Location
Our Seattle Location
Northpoint Seattle’s outpatient treatment program is located in beautiful Seattle, Washington, and we work to help the surrounding communities.
- Seattle
2111 N Northgate Way Suite 101,
Seattle, WA 98133, United States
Suboxone (Buprenorphine and Naloxone) is a medication used to help with opioid addiction recovery. Many people have had great success in using this type of medication to stop using these drugs. It helps with their cravings, and makes it easier to abstain from them.
Opioid addiction is a very real problem in the United States. In fact, according to the American Society of Addiction Medicine:
Clearly, this is a serious problem, and the hope is that Suboxone will help to solve it. If you have an addiction to opioids, you might be considering using Suboxone. It is a drug that works quite well for a lot of people. However, do you know everything about it that you should?

Suboxone is a medication that contains both buprenorphine hydrochloride and Naloxone. It may also be referred to as simply, buprenorphine, its generic name.

The Naloxone in Suboxone works by blocking the effects of opioid drugs.
The opiate blocker in Suboxone has been so beneficial to so many people. These are individuals who wouldn’t be able to stop using opioids without this drug.
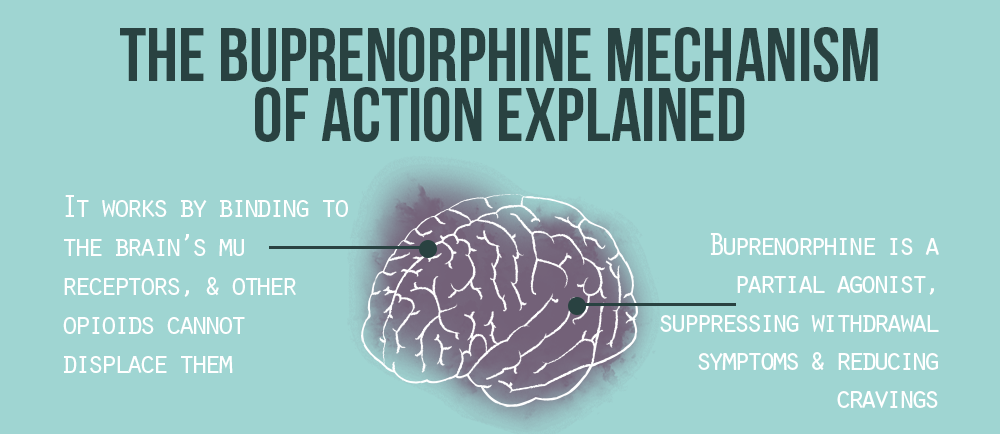
When it comes to the mechanism of action for buprenorphine, it can be explained very simply. There are receptors in the brain that are responsible for opioid intoxication. These are called the mu receptors. Buprenorphine works by binding to these receptors. No other opioids are able to displace them. This means that when a person is on buprenorphine, if they take additional opioids, the effects won’t be felt.
Also, buprenorphine is a partial agonist. This means that it does produce a slight amount of euphoria, but not much. It helps to suppress withdrawal symptoms and reduce cravings substantially.

This medication can be given to patients in brand name format or as buprenorphine naloxone, the generic form. Other names for this medication include Zubsolv and Bunavail. There are other brand names for buprenorphine, and Suboxone is only one of them.
One of the more common dosages in this format is to prescribe the sublingual tablet in 8mg/2mg. Even so, the tablets aren’t right for everyone. Suboxone is also available in sublingual strips.
If you begin to take Suboxone, sticking to your dosage is so important. This is a drug that you must take according to a strict schedule. Otherwise, you may end up abusing it, or it might not work properly for you.
Many doctors actually prefer the use of the Suboxone strips because the risk of abuse is smaller. In many parts the country, the use of the tablets is becoming obsolete.
For people using this medication appropriately, they will find quick relief from their symptoms with the strips as well. This is often another reason doctors usually recommend them over the tablets.

There is probably a lot about Suboxone that you don’t know. For example, were you aware that:
It is true that Suboxone is very controversial. Some laud it as being the answer to the opioid addiction problem in the United States. Others feel that it might only make a bad problem much worse. In many cases, it comes down to taking a risk in order to effectively treat opioid addiction.
Take an in-depth look into recovery topics with our amazing, up-to-date recovery guides.
Addiction Guides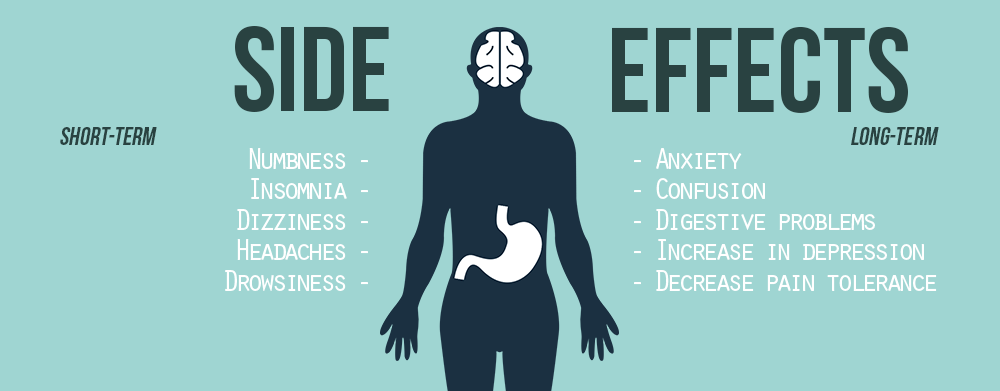
Like any prescription medication, Suboxone is going to carry side effects. This should be expected whenever you take a prescription drug. Although, sometimes the side effects from opioid drugs like this one can be worse.
Anyone who is considering taking Suboxone needs to be aware of these side effects. It may be necessary to weight the benefits of the drug against its negative impact on your body.
Naloxone can carry some serious side effects on its own. Because it is included in this drug, anyone taking Suboxone should be advised of the possible effects, which can include:
Like other forms of opioid replacement therapy, buprenorphine should not be taken long-term. Suboxone is a drug that works best when it is taken for a short period of time. It makes sense not to keep a patient on an opioid drug to replace another one long-term. Also, buprenorphine does have certain long-term effects that can be problematic.
The long-term effects of Suboxone include:
There is also a very real threat of forming a Suboxone addiction, or becoming dependent. Remember, this is a powerful drug, and it should be treated as such. Long-term use of it could have serious consequences that most people don’t count on.

When Suboxone is being taken precisely according to the prescription, there is no concern about getting high. However, a buprenorphine/naloxone high is possible when this drug is taken differently.
People who seek out the buprenorphine high are always researching the best way to experience it with Suboxone. It can produce a sensation of euphoria when it is abused.
There are different ways that you can take Suboxone to get high. Some people will just dissolve more than their usual dose under their tongue. Others will crush their buprenorphine/naloxone tablets and snort them. It is also possible to dissolve the tablets or the films and then inject them.
Buprenorphine can get high you because it is an opioid drug. This is one reason why so many are against using this medication for opioid replacement therapy.
For opioid addicts, injecting their drugs is one of the more common ways of using them. Therefore, it’s not surprising that many who choose to get high on Suboxone would try to inject it. People who choose this method of abusing Suboxone are usually surprised by the outcome.
They are expecting a strong euphoria, but that is not what they experience. The Naloxone that is in Suboxone should never be injected. When it is, it immediately puts the user into withdrawal, which can be very difficult to deal with. We’ll talk in more detail about Suboxone withdrawal symptoms in just a few minutes.
Unfortunately, buprenorphine abuse is becoming much more common with every passing year. This is because it is an opioid medication with such a high potential for abuse. People will typically take Suboxone the way that it should be taken for a period of time. After some time has passed, they will then start abusing it.
They may start to miss the feeling of being high on opioid drugs. In this case, Suboxone presents them with an opportunity to get high once again. In fact, when it comes to the buprenorphine high, Bluelight, Erowid, and other online forums have plenty of information. Many of them are people who only use Suboxone for the high it can produce.
Some experts believe that giving people Suboxone is simply trading one addiction for another. While it has been beneficial for some, one has to wonder if it’s really worth it.
It should be noted that abusing Suboxone does not mean that you are addicted to it. It is possible to abuse this drug without having an addiction. On the other hand, any abuse of buprenorphine will lead to an addiction eventually, unless it is stopped.
People can form addictions to Suboxone the same way they form them to any other opioid drug. It can happen from repeated use in some cases, but it is much more likely to happen with repeated abuse.
Even though this medication is commonly used for ORT, people tend to forget that it is an opioid. Because of this, it works in the same way that other opioids do. It attaches to the body’s opioid receptors. The result is a relief of withdrawal symptoms, the relief of pain and often, a sensation of being high.
The high feeling that addicts are always chasing is actually excess amounts of dopamine in the brain. Dopamine is the chemical the brain produces that makes people feel happy. When it is released in large amounts, it can cause euphoria.
As time goes on, and the drug use continues, the brain can lose its ability to produce dopamine without the presence of the drug. This is why people say that they don’t feel like themselves if they are not using. It is at that point that they have become addicted.
For the last few years, our country has been facing an opioid overdose epidemic that is unlike anything we have ever seen before.
The National Institute on Drug Abuse reports that every day, more than 115 people in the U.S. die as a result.
But there is no doubt that Suboxone has become a part of it. This is a crisis that is costing the United States $78.5 billion a year in healthcare costs, lost productivity, treatment and criminal justice involvement. Not to mention the number of lives being lost.
The opioid epidemic itself can be traced back to the late 1990s. Up until that point, there were fewer options for treating pain. More and more companies began to develop medications, and pharmaceutical companies assured doctors that they were non-addictive. Doctors believed them and began prescribing them often. After all, they were perceived to be safe, and they were very effective as well.
The result was the widespread use, misuse and diversion of these drugs. Once they became more difficult to get, people started turning to heroin to get high instead. The number of people overdosing on these drugs steadily increased. In 2015, there were more than 33,000 Americans who died from overdosing on opioid drugs. During that same year, around 2 million people were suffering from a substance use disorder that was related to opioid medications.
The unfortunate answer to this question is no; most doctors are not equipped to handle the opioid epidemic and all that it entails.
The New York Times published an article on their website that details this quite clearly. It tells the story of a case study that was presented to a medical student. The patient was suffering from residual leg pain from an older injury. He was requesting a stronger opioid, even though he had already been given Percocet. The patient tested positive for two other drugs, including hydromorphone, which is a very powerful painkiller. The doctors had not ordered it for him. In addition, he did not test positive for Percocet.
The medical student had no idea how to have a conversation with this patient about his test results. It was obvious that he was abusing the hydromorphone, but the up and coming doctor did not know what to say.
The reality is that it can be hard for doctors to tell the difference between extreme pain and drug dependence. But they are on the front lines of intervention. By and large, it is up to them to determine whether or not a patient has become dependent on an opioid drug. This includes patients who are taking Suboxone.
Addiction is not a subject that is addressed enough in medical school. The National Center on Addiction and Substance Abuse at Columbia University cites the failure of the medical profession at every level to address it the correct way.
NIDA reports that in 2016, more than 11 million people in the United States misused prescription opioids. That’s only one year. The total number is astronomical. Clearly this is an issue that needs to be addressed.
The President has called the opioid crisis a national health emergency, and it should be treated as such. The Department of Health and Human Services has put a five-fold plan in place to attack the issue head-on. The plan states:
Research into better methods of managing pain and treating addictions is so important during this critical time in our nation’s history. Fortunately, that research is being done.
At the Wake Forest School of Medicine, scientists believe that they may have found the answer for the opioid crisis. They have discovered a new compound that has the ability to treat pain and reduce the effects of opioids that cause them to become addictive. The compound is being referred to as AT-121.
They study was done in primates, and the AT-121 showed the same level of pain relief that opioid drugs provided. Interestingly enough, it performed well at a dose that was 100 times lower than morphine.
It is believed that once AT-121 becomes a drug, it could completely eliminate the need for Suboxone. But getting it into the public’s hands is a long ways away. There are still more trials to conduct, and the FDA needs to be petitioned before they can conduct clinical trials in humans. The entire process could take as long as seven years to complete, but there is hope.
There are actually several other drugs that can be used during opioid replacement therapy. Suboxone is only one of them. It’s interesting to take a look at how buprenorphine measures up against the others.
Suboxone vs. Subutex are two medications that are frequently compared with each other. People are usually told that they have two different options, and both are close to being equally beneficial.
This is partially true. Suboxone and Subutex are very similar to each other. However, Subutex does not contain Naloxone. This is the main difference between the two of them. Both contain buprenorphine, which is eventually converted into norbuprenorphine in the liver.
People will frequently begin recovery with Subutex, and then switch to Suboxone. Even so, the price may be enough to keep people on Subutex longer. A 30-day supply of Subutex ranges from $45 to $110, whereas for Suboxone, it costs between $128 and $470.
As we’ve previously discussed, Naloxone is a drug that is a part of Suboxone. Still, people wonder if the buprenorphine component of Suboxone is really necessary.
On its own, Naloxone is frequently given as a drug. Sometimes it goes by the name, Narcan. Narcan is better suited in situations of possible opioid overdose when it is used on its own. Naloxone is helpful for neutralizing all of the opioids a person has taken. It will actually travel to a person’s opioid receptors and remove any opioids that are there.
It makes sense why Naloxone is a part of Suboxone. However, it’s also easy to see why this wouldn’t be quite as effective in ORT on its own. This is why it’s not prescribed for this purpose.
You may not realize that buprenorphine and subutex are actually the same thing. Buprenorphine is also found in Suboxone, as we have previously discussed. Some experts believe that the risk of addiction might be lower with buprenorphine alone than it is with Suboxone.
Patients who have used both also claim that Suboxone caused them to feel sad and depressed. Buprenorphine did not.
Methadone vs. buprenorphine are also frequently compared to one another. At one time, methadone was the primary drug of choice for opioid replacement therapy. It is also effective at treating pain. Still, those in the addiction treatment field felt that it needed some improvements.
Methadone can treat opioid dependence, as well as chronic pain. However, it is a drug that must be highly controlled. It can only be given in methadone clinics. The potential for abuse and addiction to methadone is much higher than it is for buprenorphine.
One major difference and advantage of methadone is that it has fewer side effects. Still, most people believe that the benefits of buprenorphine outweigh those of methadone.
Taking methadone and buprenorphine together is never recommended. There are cases when people have a desire to get off methadone because it is so highly addictive. In that case, they may be recommended for either Subutex or Suboxone. Even so, they will need to be weaned off very slowly. They may also need to be off it completely before the buprenorphine medication can be started. Otherwise, they may experience symptoms that mimic opioid withdrawal.
Naloxone pentazocine is a medication that is usually used to treat pain. It really isn’t effective at all as a form of opioid replacement therapy. The pentazocine in the medication is an opioid drug, and the naloxone is used to keep it from becoming addictive.
If Naloxone pentazocine is misused or abused, it can result in death. Therefore, it might not be a good idea to give this medication to someone with a history of opioid abuse. In this case, Suboxone would be a much better choice.
Vivitrol is one of the newest drugs on the market that is being used to treat opioid addiction. The earliest results of its use are quite promising, and there have been many people who have recovered well.
When comparing Vivitrol vs. Suboxone, researchers found both drugs to be equally effective at treating opioid addiction. But there are some differences in the way the medications are administered.
Vivitrol’s generic name is naltrexone. It is given in the form of an injection that lasts for 30 days. Because of this, it is often favored by doctors who do not want to leave medications in the hands of patients with histories of addiction.
The best part about Vivitrol is that it is not an opioid drug at all. In fact, it does not have any addictive qualities whatsoever. This in itself makes it a prime candidate for treating people who are addicted to painkillers and other opioids.
One of the issues with Vivitrol is that it cannot be given to patients immediately the way that Suboxone can. Those who take it need to go through a period of detoxification first. This can be problematic, and it can be very difficult for them to manage their withdrawal symptoms during that time. Many doctors feel that this presents a significant barrier to treatment.
Still, many treatment programs are beginning to offer Vivitrol services to their clients. It is a drug that is worth considering because it appears that people have a high rate of success with it.
Most doctors adhere to the principle of starting their patients on Subutex and then moving them to Suboxone. However, there are those who do the exact opposite. This is interesting because with Subutex, the absence of Naloxone allows people to feel the effects of buprenorphine. In a way, moving their patients to Suboxone afterwards is almost like weaning them off the buprenorphine.
So, the question is, why would a doctor want their patients to go back to experiencing those opioid effects? It actually isn’t for the buprenorphine euphoria, although this experience could occur.
Also, switching from Suboxone films to Subutex tablets could be problematic for another reason. With the films, the medication is dissolved easily under the tongue. With the tablets, they are more likely to be swallowed, which means getting less of the medication.
Take one of our addiction quizzes to find out if you or someone you care about needs help today.
Under the most perfect of circumstances, patients are kept on Suboxone or buprenorphine short-term. They may take these medications for around two months, and then stop. Patients taking Suboxone are frequently kept on it for much longer than that.
Suboxone dependence is likely to develop with long-term use. When it does, it is necessary to stop taking this drug. The Buprenorphine half-life is between 3 hours and 37 hours, depending on how you take it. That means it takes that amount of time for half of the drug to leave the body. Once it starts to leave the body, withdrawal symptoms will begin if you are dependent.
Suboxone withdrawal is not easy to go through. In fact, for many people, it actually requires professional treatment through drug detox.
If you have become dependent upon Suboxone, stopping it will result in withdrawal symptoms. You should expect to experience:
Generally, symptoms start off being mild, and then escalate in their severity. People usually experience a peak right around day 3. After that, symptoms start to get better. However, it can take a few weeks before full relief is felt.
When people begin taking buprenorphine, they never think about the possibility of becoming an addict. Most people take Suboxone because they want to get help with their opioid addictions. Unfortunately, they often get much more than they had bargained for.
You may not realize that you have gotten addicted to buprenorphine right away. In fact, it could take months before you start to feel the effects of this addiction. Still, with this medication, an addiction to Suboxone is a very real possibility. That means you need to know what to look for and how to identify it.
You may want to think about taking an addiction quiz. That will answer many of the questions you have about your Suboxone use. You could also look for some of the following symptoms and signs of buprenorphine addiction:
Yes, it is possible to overdose on Suboxone, and there are a lot of people who do. In fact, this medication is being found at many scenes of overdose victims. The drug is showing up in their toxicology reports, which shows that there is real reason for concern.
Dr. Darinka Mileusnic-Polchan, who is a Medical Examiner states that Suboxone is normally not deadly on its own. However, that changes when it is combined with other opioid drugs or any illicit substance at all.
It does not help that patients in hospitals are frequently given opioid drugs to treat pain. Many aren’t even questioned about whether or not they are on any other type of medication. In a lot of cases, the patient’s use of Suboxone is never even mentioned.
When patients start taking this medication, they are given information about it. The PDF they receive states that:
“Suboxone Film can cause serious life-threatening breathing problems, overdose and death, particularly when taken by the intravenous (IV) route in combination with benzodiazepines or other medications that act on the nervous system (ie, sedatives, tranquilizers, or alcohol). It is extremely dangerous to take nonprescribed benzodiazepines or other medications that act on the nervous system while taking Suboxone Film.”
It is important to note that an opioid overdose is not something that people can just sleep off. This is an emergency situation, and quick action must be taken in order to save the person’s life.
You should know what the signs of an opioid overdose are. They include:
If you suspect that someone you love has overdosed on Suboxone either on its own or in combination with other substances, please act quickly. Do not attempt to take them to the emergency room on your own. Instead, call 911. Inform the paramedics of your suspicion of an overdose. They should be able to administer life-saving medications right there at the scene.

This is a very good question, and it’s one that you need to get an answer to. At Northpoint Seattle, we want you to get the answers you need. It’s possible that Suboxone might very well be an excellent option for you if you need opioid replacement therapy. However, it is also possible that alternate methods of treatment might work just as well, if not better.
There are different medications you can take, that aren’t opioid drugs. There are also holistic methods of detox that don’t use any medications whatsoever. The most important thing you can do is to find the method that will work the best for you.
We want to help you find the information you’re looking for. Do you have additional questions about whether or not Suboxone is right for you? If you do, we’d like to help you as much as we can. Please contact us to learn more.

Our admissions coordinators are here to help you get started with treatment the right way. They'll verify your health insurance, help set up travel arrangements, and make sure your transition into treatment is smooth and hassle-free.
888.483.6031Contact Us